The procedure usually takes around 10 minutes, but this can vary depending on how twisty your bowel is and if we need to do anything extra such as polyp removal.
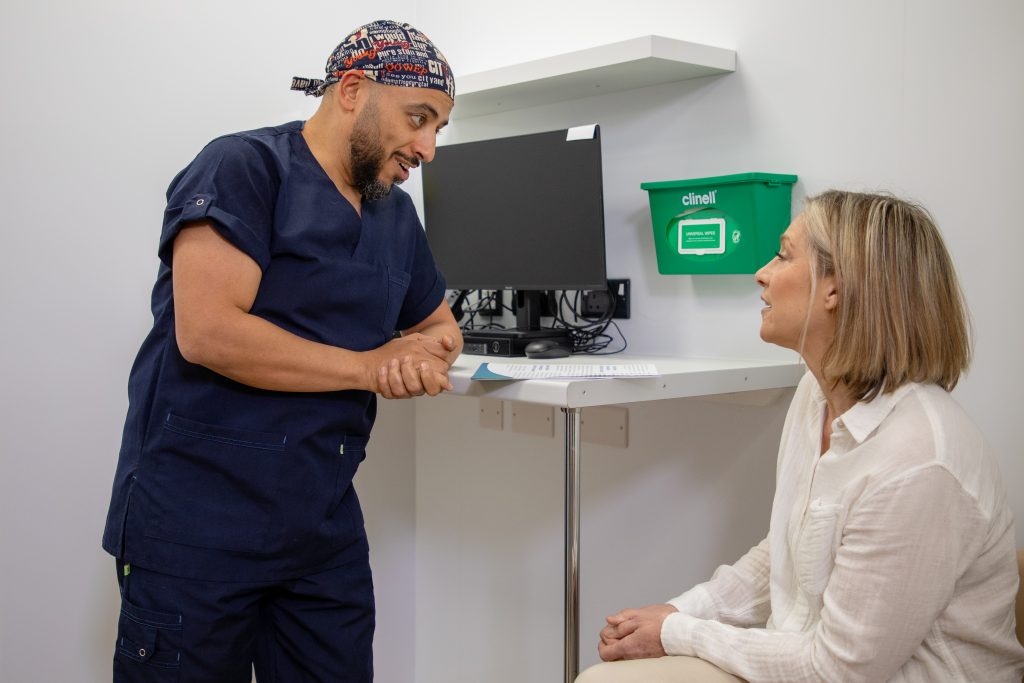
Flexible sigmoidoscopy is a quick test, and most people are perfectly comfortable without any sedation or painkillers. If you’re feeling particularly worried about it, our friendly hospital team are on hand and they’ll be happy to help answer any questions you may have.
While you are preparing for your flexible sigmoidoscopy here at Clarity, it’s a good idea to keep to a healthy diet, cut back on alcohol, and think about giving up smoking if you currently smoke.
Try and avoid being too constipated by using laxatives regularly if you suffer with constipation. This will also really help make sure your bowel is properly emptied out when you take the bowel prep before your appointment.
Avoid foods that make your bowel symptoms worse.
It is extremely important that the left side of your bowel is completely empty before a flexible sigmoidoscopy to allow adequate inspection of the lining of your colon.
Once your sigmoidoscopy is booked in, you will receive detailed instructions on how to prepare for you appointment. Usually, this involves taking a bowel-cleansing laxative at home the day before your procedure. Sometimes, all that’s needed is an enema on the day of the test; we’ll let you know if that’s the case.